Cardiovascular disease and musculoskeletal conditions – Professor Maya Buch speaks to Arthritis Digest
Arthritis Digest is a magazine for people with arthritis that highlights the latest relevant research and reviews topical issues. With researchers from Manchester BRC’s Musculoskeletal theme contributing articles throughout 2020, Maya H Buch, Professor of Rheumatology, starts 2021 with a look at the links between cardiovascular disease and rheumatic and musculoskeletal diseases.
Heart Matters – Our understanding of the links between cardiovascular disease and rheumatic and musculoskeletal diseases is improving outcomes for patients, explains Prof Maya Buch.
Cardiovascular disease (CVD) means disorders of the heart and circulatory system (blood vessels) and is common in the general population. CVD includes:
- Coronary artery disease (furring up of the arteries that supply the heart), which causes chest pain symptoms when the heart needs to pump harder, for example, during exercise. This is common and can lead to heart attack;

- Heart attack when blood supply to the heart is blocked;
- Heart failure when the heart is unable to pump blood to the rest of the body properly;
- Disease of the heart muscle (cardiomyopathy) making it
CVD and rheumatic and musculoskeletal disease
People with rheumatic and musculoskeletal diseases such as rheumatoid arthritis, systemic lupus erythematous, systemic sclerosis, and vasculitis have an increased risk of CVD.
The type of CVD seen in each disease can vary. For example, people with rheumatoid arthritis and lupus experience more heart attacks and heart failure. People with systemic sclerosis and lupus may also suffer from cardiomyopathy with inflammation of the heart muscle, heart rhythm or conduction abnormalities (the electrical impulses that travel through your heart) and heart failure.
While the type of CVD may be different, we know that in addition to traditional risk factors (such as diabetes, high blood pressure, high cholesterol, smoking, being overweight and family history), the rheumatic and musculoskeletal diseases themselves increase risk of CVD.
This is because the inflammation processes and the immune systems of people with these diseases also affects systems such as the heart and vessels. The exact mechanisms, however, are still unclear.

What is being done to tackle CVD in these groups?
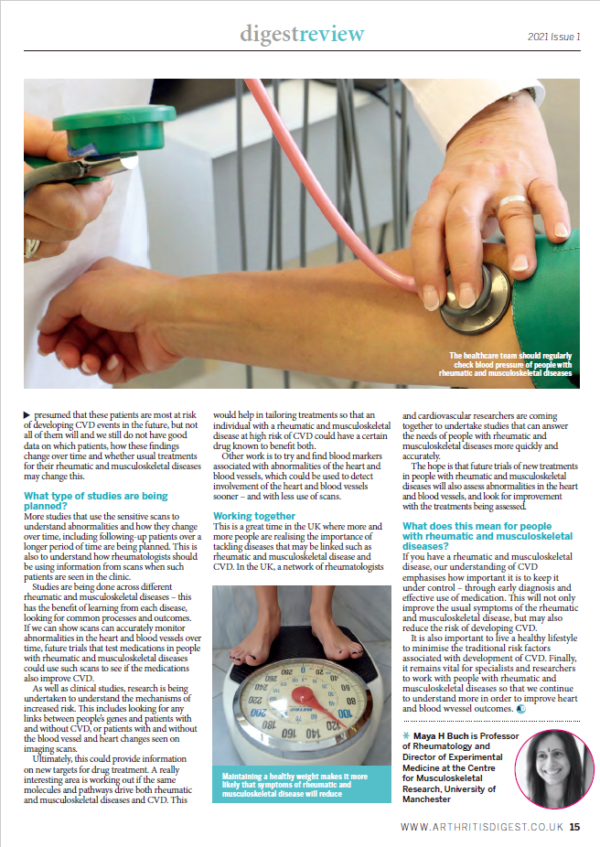
We know it is vital to control traditional risk factors (i.e. give up smoking, lower blood pressure and cholesterol if need be and maintain a healthy weight). Rheumatologists keep an eye on this and communicate with the patient’s GP to ensure regular blood pressure checks and blood tests are performed to pick up risk factors that need medication and monitoring. Smoking cessation programmes are very important.
Some departments bring together cardiology and rheumatology specialists in order to discuss and manage patients more effectively.
However, we need to understand who is at most risk most, how best to pick up heart and blood vessel involvement early, and what treatments can reduce the risk. Because of the link between inflammation and CVD, a lot of research is focusing on whether treatments typically used for rheumatic and musculoskeletal diseases (and maybe new medication that target inflammation) may also help the heart and blood vessels.
What does the research say?
A challenge in studying people with rheumatic and musculoskeletal diseases and possible treatments to reduce heart attacks, heart failure and stroke, is that a lot of patients need to be recruited and followed up over a long period of time to pick up these events.
Instead, tests that can serve as an indicator of CVD can be used. A lot of research over the last 10 years (*1,2,3) has taken advantage of imaging tools, such as computerised tomography (CT) scans and magnetic resonance imaging (MRI) scans, to identify people with rheumatic and musculoskeletal diseases who are at risk of CVD and how this may change over time. These scans are very sensitive at picking up changes in the vessels and the heart.
Many researchers have performed such scans on people with, for example, rheumatoid arthritis, who have no known history of heart disease and found signs of abnormalities in the heart and blood vessels. This has been shown even at the earliest stage of disease, at time of diagnosis.
Interestingly, studies have shown that treatments used for rheumatoid arthritis can improve these abnormalities, regardless of how much the treatment improved people’s arthritis symptoms. This suggests that in addition to suppressing inflammation, treatments for rheumatoid arthritis might influence risk of CVD by other means, maybe by directly changing underlying processes of heart and vessel disease.
Other studies (*4,2) in people with lupus and systemic sclerosis have shown a large proportion have evidence of inflammation and scar of the heart muscle without any symptoms. It is presumed that these patients are most at risk of developing CVD events in the future, but not all of them will and we still do not have good data on which patients, how these findings change over time, and whether usual treatments for their rheumatic and musculoskeletal diseases may change this.
What type of studies are being planned?
More studies that use the sensitive scans to understand abnormalities and how they change over time, including following-up patients over a longer period of time are being planned. This is also to understand how rheumatologists should be using information from scans when such patients are seen in the clinic.
Studies are being done across different rheumatic and musculoskeletal diseases – this has the benefit of learning from each disease, looking for common processes and outcomes. If we can show scans can accurately monitor abnormalities in the heart and blood vessels over time, future trials that test medications in people with rheumatic and musculoskeletal diseases could use such scans to see if the medications also improve CVD.
As well as clinical studies, research is being undertaken to understand the mechanisms of increased risk. This includes looking for any links between people’s genes and patients with and without CVD, or patients with and without the blood vessel and heart changes seen on imaging scans.
Ultimately, this could provide information on new targets for drug treatment. A really interesting area is working out if the same molecules and pathways drive both rheumatic and musculoskeletal diseases and CVD. This would help in tailoring treatments, so that an individual with a rheumatic and musculoskeletal disease at high risk of CVD, could have a certain drug known to benefit both.
Other work is to try and find blood markers associated with abnormalities of the heart and blood vessels, which could be used to detect involvement of the heart and blood vessels sooner – and with less use of scans.
Working together
This is a great time in the UK where more and more people are realising the importance of tackling diseases that may be linked, such as rheumatic and musculoskeletal disease and CVD. In the UK, a network of rheumatologists and cardiovascular researchers are coming together to undertake studies that can answer the needs of people with rheumatic and musculoskeletal diseases more quickly and accurately.
The hope is that future trials of new treatments in people with rheumatic and musculoskeletal diseases will also assess abnormalities in the heart and blood vessels, and look for improvement with the treatments being assessed.
What does this mean for people with rheumatic and musculoskeletal diseases?
If you have a rheumatic and musculoskeletal disease, our understanding of CVD emphasises how important it is to keep it under control – through early diagnosis and effective use of medication. This will not only improve the usual symptoms of the rheumatic and musculoskeletal disease, but may also reduce the risk of developing CVD.
It is also important to live a healthy lifestyle to minimise the traditional risk factors associated with development of CVD. Finally, it remains vital for specialists and researchers to work with people with rheumatic and musculoskeletal diseases so that we continue to understand more in order to improve heart and blood vessel outcomes.
1. Fent GJ, Greenwood JP, Plein S, Buch MH. The role of non-invasive cardiovascular imaging in the assessment of cardiovascular risk in rheumatoid arthritis: where we are and where we need to be.
2. Plein S, Erhayiem B, Fent G, Horton S, Dumitru RB, Andrews J, Greenwood JP, Emery P, Hensor EM, Baxter P, Pavitt S, Buch MH. Cardiovascular effects of biological versus conventional synthetic disease-modifying antirheumatic drug therapy in treatment-naïve, early rheumatoid arthritis.
3. Bissell LA, Erhayiem B, Fent G, Kidambi A, Swoboda P, Abignano G, Donica H, Burska A, Greenwood JP, Biglands J, Del Galdo F, Plein S, Buch MH. Predictors of subclinical systemic sclerosis primary heart involvement characterised by microvasculopathy and myocardial fibrosis.
4. Lea Winau,rocio Hinojar Baydes,Axel Braner,Ulrich drott,Harald Burkhardt, Shirish Sangle,david p d’Cruz,Gerry Carr-White, Mike Marber,6 Katrin SchnoesChristophe Arendt, Karin Klingel, thomas J Vogl, Andreas M Zeiher, Eike nagel, Valentina o puntmann. High-sensitive troponin is associated with subclinical imaging biosignature of inflammatory cardiovascular involvement in systemic lupus erythematosus.